EXCELLENTTrustindex verifies that the original source of the review is Google. Excellent care and level of expertise. I had titanium implants removed and a large cavitation treated. The doctor was excellent and advised for what was best for me. Will return for future treatments.Posted on GoogleTrustindex verifies that the original source of the review is Google. Hayatımda ilk defa hastasıyla bu kadar ilgilenen, bu kadar özenen, anne şefkatiyle diyeceğim, çalışan bir diş hekimi görüyorum. Memnun kalmaktan çok başka bir his. Güven duyuyorum Tuğba hocama. İnsan bedenine en uyumlu malzemeyi, en zararsız tekniği seçen, işinde son derece profesyonel bir hekim. Biyolojik diş hekimi, holistik diş hekimi, bütüncül diş hekimi diye isimler verebiliriz kendisine ama en önemlisi insan sağlığını korumaya odaklanmış, “dürüst” hekim olması.Posted on GoogleTrustindex verifies that the original source of the review is Google. I had an incredible experience with Dr. Tugba Duymaz. I was nervous about my Sinus Lifting procedure, but the entire team was professional, kind, and supportive throughout the process. The surgery went smoothly, and I was amazed at how fast my recovery was (10 days)—much quicker than I expected! I also had my teeth cleaned with ozone by Dr. Senanur, and it was such a refreshing and gentle experience. I could tell they really prioritize holistic care and overall well-being of their clients. If you’re looking for a skilled, compassionate holistic dentist who uses advanced techniques and truly cares about their patients, I recommend Dr. Tugba Duymaz, she and her team provide exceptional care!Posted on GoogleTrustindex verifies that the original source of the review is Google. Tuğba Hanım'ı bütünsel ve koruyucu tıp okumalarım sırasında keşfetmiş ve tam aradığım diş hekimi diye düşünmüştüm. Önce muayene, ardından diş temizliği uygulaması için gittim. Gerek kendisi gerek kliniğindeki tüm çalışanlar (eşi Oktay Bey'in profesyonel beceriyle katkısı ayrıca övgüye değer), "kaliteli sağlık hizmeti"nin tüm parametrelerini taşımaktalar. Bu harika ekibi yürekten kutluyor ve teşekkür ediyorum.Posted on GoogleTrustindex verifies that the original source of the review is Google. I am incredibly grateful to have found Dr. Tugba Duymaz, as this has been the best dental experience I've ever had. From my very first contact with the team, I received highly professional treatment, and as a completely new patient, I was provided with all the desired details and information. All preparations for the appointment and treatment were meticulously planned. After my initial consultation with Dr. Duymaz, I felt completely confident that my planned implant surgery would be successful. And indeed it was - the operation went smoothly, and I experienced no pain afterward. Compared to my previous implant experience, the difference is night and day. The entire team is extremely friendly and empathetic. Most importantly, they take ample time with each patient rather than rushing through procedures at the expense of quality - something that seems almost miraculous to find in today's fast-paced world. I can highly recommend this practice to international patients as well, as their appointment scheduling is perfectly coordinated. I'm already looking forward to my next visit to complete my treatment! :-)Posted on GoogleTrustindex verifies that the original source of the review is Google. An extremely nice and pleasant experience with Dr. Duymaz and her team!!!! Starting with first contact I had with the team I was treated very professional and received all details requested as a completely new patient. So I am extremely and positively surprised by the good preparation when onboarding a new customer with Dr. Duymaz cabinet. All preparations for the appointment and treatment were done very carefully and after having my first appointment and consultation with Dr. Duymaz I was fully confident that my surgery for the implant I planned will be a success. Even if I had some fears regarding the procedure and pain to expect after the surgery, I can tell pain was none (during and as well after the procedure) Beside her professional skills, Dr. Duymaz is a very kind and empathic person who took the necessary time to go with me through the stages of the treatment as well as paying the attention needed to the details in order to assure me the confort I was looking for related to the upcoming surgery. A pleasure to meet such a professional team. So definitely recommend at least one appointment with Dr. Duymaz, the rest will come naturally on its own and I am absolutely confident you will discover that the facts described in this review are genuine. Congratulations to YOUR professionalism and your dedication Dr. Duymaz -yours and your entire team!Posted on GoogleTrustindex verifies that the original source of the review is Google. Sena hanım amalgam sökümü, diş temizliği ve diş beyazlatma işlemlerimi gerçekleştirdi. Özenli bir şekilde çalıştı ve beni güzelce bilgilendirdi. Sonuçlardan memnun kaldım. Tekrar tercih edeceğim bir klinik kesinlikle.Posted on GoogleTrustindex verifies that the original source of the review is Google. So far, I'm extremely grateful that I've found Dr. Tugba. I had some significant nerve pain and also an infection in one of my teeth, and have gotten two different opinions from conventional dentists and they immediately resorted to root canal treatment, a treatment I was very opposed to. After finding Dr. Tugba and reading her biography, I reached out. She performed root capping and ozone gas treatment and did a procedure on an extremely sensitive tooth, which was a difficult position to be in. Although it's still early to know with certainty whether or not the tooth has been saved, the reduction in pain and sensitivity makes me hopeful and optimistic that it is. I look forward in having a long lasting relationship with Dr. Tugba as we work together to repair all the dental issues I'm having.Posted on GoogleTrustindex verifies that the original source of the review is Google. I found Dr Tugba Duymaz online as I was looking for a biological dentist to sort out a host of issues with my teeth. My treatment journey with Dr Tugba that started in early 2023 has just ended in November 2024. I cannot say how truly grateful I am for the care and diligence she has shown towards my treatment. She is patient and takes time to answer all questions, especially for anxious patients such as myself. And my experience is that she truly takes the time to do a good job. My treatments have included ozone gas and PrP, and I have not had any challenges with pain or infection over the many procedures I have had. Not even in my injection sites which were such a problem with previous dentists. I could go on for much longer, but I will not, though I wanted to show my deepest appreciation for Dr Tugba. Also for the kind assistance of Oktay Duymaz ensuring I had the support I needed for my Visa applications and numerous appointments. My thanks too to the rest of the staff who are extremely kind and professional. THANK YOU!!!Posted on GoogleTrustindex verifies that the original source of the review is Google. Kendinizi hem bir biyolojik diş hekimine, hem de nazik bir sanatçının ellerine bırakmak istiyorsanız doğru yerdesiniz. Tuğba Hanım’la bir blogta bir ropörtajı vesilesiyle tanışmıştım, eğer bir gün bir diş hekimine gitmem gerekirse mutlaka Tuğba Hanım olmalı demiş sonrasında amalgam dolgularımın sökümü için kendisine başvurmuştum. Türkiye’de bildiğim kadarıyla Smart protokolünü uygulayan nadir hekimlerden birisi ve bunu öyle ustaca yapıyor ki kendisine hayran kalmamak elde değil. Kompozit dolgularımı ve diş taşı temizliğimi her seferinde sabırla ve özenle yaptı. Her alanda kendisini sürekli geliştirdiği ve hastalarına holistik bir yaklaşımla destek verdiği için minnetarım. Diş tedavisi deneyimini bambaşka bir noktaya taşımış kendisi. Her şey için tekrardan teşekkürler.
We believe that dentistry is not just about treating teeth and gums, but about developing a harmonious relationship between oral health and our overall health. For this reason, we have committed ourselves to the principles of “holistic dentistry“, which acts with the awareness of the connection between oral health and body health and emphasizes the importance of this connection. For this reason, our priority in our treatments is to detect the presence of problems in your mouth that may affect your general health, to give priority to biocompatible materials and minimally invasive techniques in solving them, to act with approaches that aim to preserve the vitality of teeth such as “biomimetic dentistry” and to benefit from systemic supports while doing so.
MEMBER OF
Ceramic/Zirconia Implants
Since ceramic implants do not corrode like metals, they are more tissue-compatible, and they also enable more aesthetic results, especially in the anterior region. Before the application of ceramic implants, the patient should be prepared for surgery with the correct protocols.
SMART | Safe Amalgam Removal
The SMART amalgam removal protocol determined by the International Academy of Oral Health and Toxicology (IAOMT) is implemented with all necessary equipment.

IAOMT Ambassador of Turkey

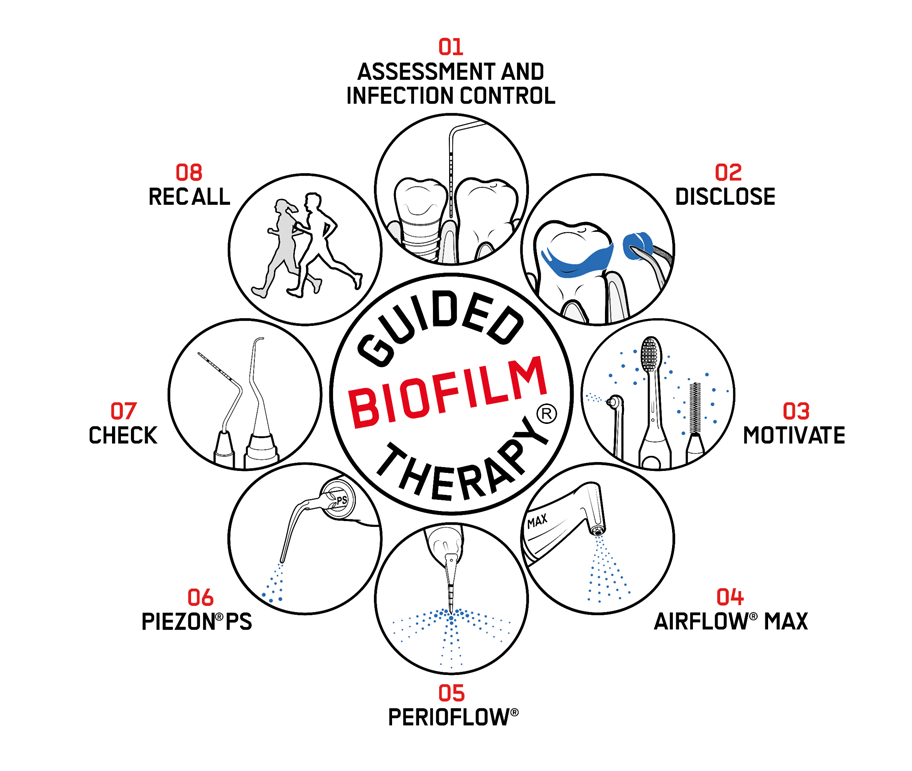
Guided Biofilm Therapy(GBT)
The goal of guided biofilm therapy (GBT), a cutting-edge method of oral hygiene and dental care, is to effectively remove dental biofilm and stains. To ensure ideal dental health, it blends cutting-edge technology, evidence-based practices, and thorough treatment. GBT places a strong emphasis on creating individualized treatment regimens that are suited to the needs of each patient. To effectively and delicately remove biofilm, plaque, and surface stains from teeth and soft tissues, GBT uses methods including air polishing and ultrasonic scaling. This methodical and minimally intrusive technique promotes a bright, clean, and healthy smile while improving overall dental wellness. It also helps prevent and treat oral disorders.



PRF
PRF (platelet-rich fibrin) is a method used in surgeries in the mouth area, implant operations, gingival problems and healthier recovery of extraction cavities.
Ozone Applications
I use ozone in the clinic from tooth extraction to cleaning of the implant and NICO areas in all bleeding procedures, caries, advanced gum diseases, canal treatments and many more.
NICO
Although NICO means neuralgia, that is, dead areas in the jawbone that cause nerve-induced pain, in some patients it can creep in the bone without any symptoms.
Biocompatible Materials
In my clinic, I take care to use biocompatible materials instead of metals that contain metals such as nickel, chromium, and cobalt and can pass through to the surrounding tissues and body through corrosion.

Tooth Extraction
Tooth extraction may cause problems in the future if the body does not have an ideal environment for bone healing. Therefore, there are some precautions that can be taken before and after tooth extraction.
Holistic Oral Examination
We cannot treat oral and dental problems as if they are problems specific to the mouth, independent of general health. Problems in the mouth can both point to other problems in the body and can be the cause of these problems!

Invisalign / Clear Aligners
At our clinic, Dr. Şahin Barış leads orthodontic treatments using Invisalign clear aligners due to their high biocompatibility. Based on rigorous testing of the raw materials and manufacturing processes, Invisalign aligners and retainers are free from latex, parabens, phthalates, glutaraldehyde, epoxy, and Bisphenol A (BPA), making them a safe and health-conscious choice for our patients.







